Your Brain Can Heal Your Body
Let us show you how with the only science-backed brain retraining program for chronic conditions.

Ashok Gupta has featured on:

Gupta Program™ Brain Retraining is a powerful revolutionary Neuroplasticity, Somatic Retraining, Limbic Retraining & Holistic Health Program for Chronic Conditions, including Long Covid
Do you have any of the following conditions?
Neuro-Immune
and many others
Environmental
and many others
Thousands of people have healed before you, and you can too.
The Gupta Program is the first brain retraining app that uses a package of proven techniques to help you recover from chronic health conditions.
Our comprehensive range of unique techniques rewire the brain and reverse your symptoms using the power of neuroplasticity – a hot new topic in medicine which is transforming lives worldwide.
Meet our Founder, Ashok Gupta
I Healed And So Can You
I suffered from ME/CFS myself and I managed to recover fully, for which I am so grateful. I’ve made it my life long quest to help others like you recover too, from similar chronic conditions.
My 25 years of research combined with the latest findings about “neuroplasticity”, lead me to believe these conditions are ultimately caused by abnormalities in brain function, which can be reversed using revolutionary “brain retraining” techniques, called “Amygdala and Insula Retraining”.
Despite what people may say, many people do recover successfully from these conditions, and the Gupta Program triggers the body’s natural ability to heal itself.

Real Retrainers. Real Stories. Real Recovery.





Hear From Medical Experts
The Science
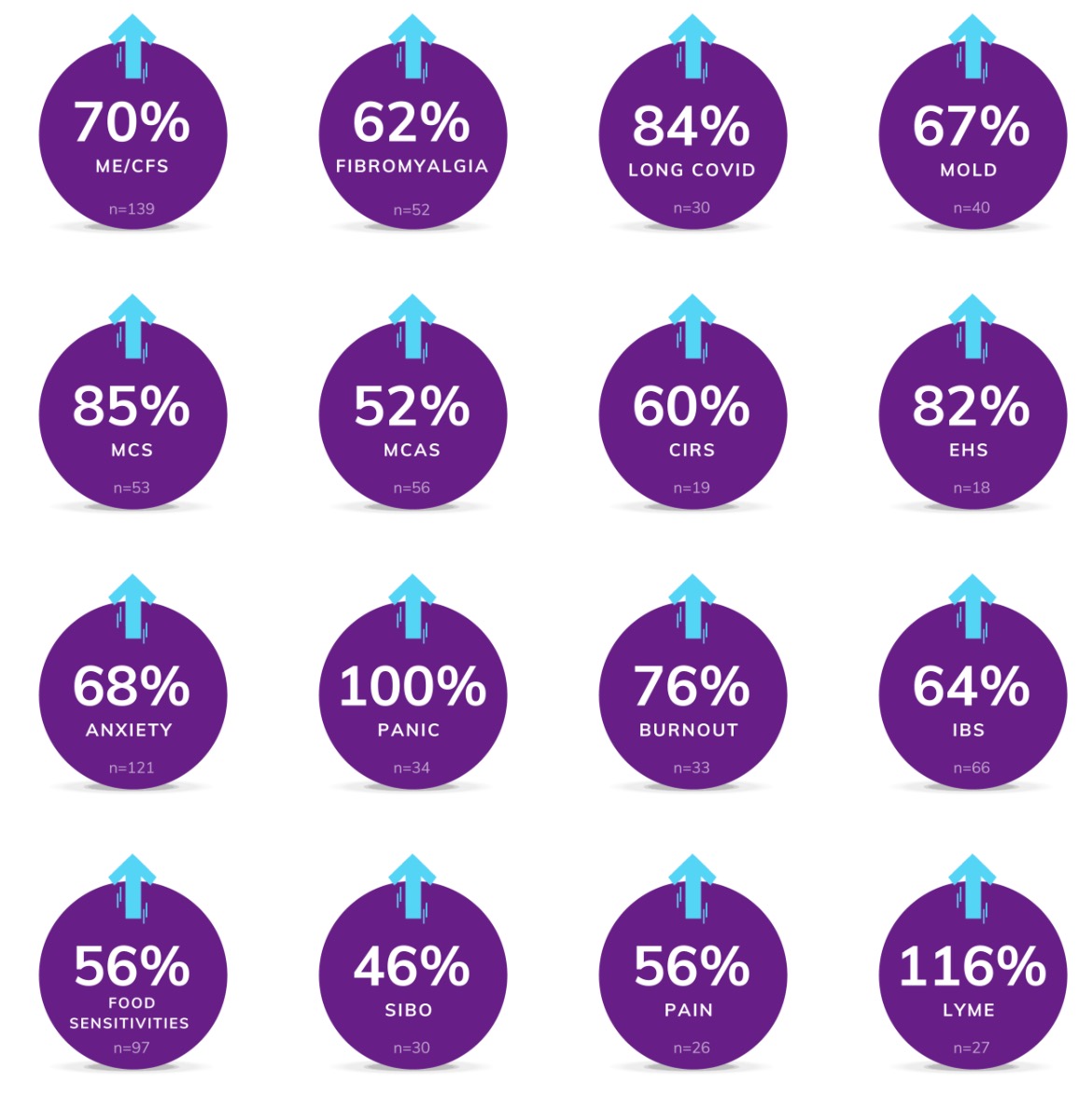
The Gupta Program has been shown to reverse symptoms across many health conditions in several peer-reviewed randomized controlled trials and clinical audits. Below is the percentage improvement in symptoms and function after 3 months on the Gupta Program in a recent published study:
Answers to your questions
The free trial gives you access to the first three modules of the program for one month, so that you can see if the program feels like the right fit for you. A subscription provides you with access to the complete program for one-year.
You can download the app from the App Store on iPhone or the Google Play Store on Android.
You can access the program via the app on any device that supports app installations. Alternatively, you can access it with your login through the website.
Many chronic conditions start in the brain, including those related to an overactive amygdala. When faced with a threat like a virus, stress, trauma, or something else, the brain sends danger signals to the body. But for some people, these signals carry on after the threat has gone, causing symptoms that can be addressed through techniques like amygdala retraining and brain rewiring programs.
The good news is that the brain is always changing and adapting. Through brain retraining exercises, such as amygdala retraining and brain rewiring programs, we can guide it back into a state of safety, reversing the symptoms associated with an overactive amygdala. This is the power of neuroplasticity; a hot new topic in medicine which is transforming lives worldwide.
Limbic system retraining focuses on resetting the brain's emotional center to alleviate symptoms of chronic conditions and improve overall well-being.
By incorporating limbic brain retraining techniques, such as amygdala retraining and brain rewiring programs, into daily routines, individuals can experience improvements in their health and quality of life.
Limbic brain retraining techniques, can be beneficial for individuals looking to address issues related to the limbic system, such as stress, anxiety, and chronic health conditions.
We understand starting a new journey can feel daunting, but rest assured, the Gupta Program is crafted to ease you into the healing process gently. We’ve organized the program into manageable steps, allowing you to learn and heal at your own rhythm, with a compassionate community and dedicated coaches to support you. You can also tailor the program to your individual pace and preference.
Our program is not just about healing; it’s about creating a supportive environment to keep your spirits high. With daily ‘Guptacise’, our caring community, and Coaches who are here for you, we will lift you up. Your journey is our journey, and together, we will maintain the momentum towards your recovery.
Our methods are grounded in science and the program is proven to be effective across many different conditions. It is natural for you to question new approaches, especially after many attempts at healing. This is why we open our doors to you with a free trial, inviting you to experience the program’s potential, including daily ‘Guptacise’ healing sessions, with no obligations.


























































